For cancer patients, living a life with and beyond cancer faces various challenges. Consider physical illness, emotional pain, financial cost, and psychological burden, etc.
Here is good news for those who are not aware of new cancer treatment program.
To improve cancer care and reduce the cost, Center for Medicare and Medicaid Services (CMS), particularly its Innovation Center (CMMI), developed Oncology Care Model, which are participated by over 190 health care providers and some insurance companies.
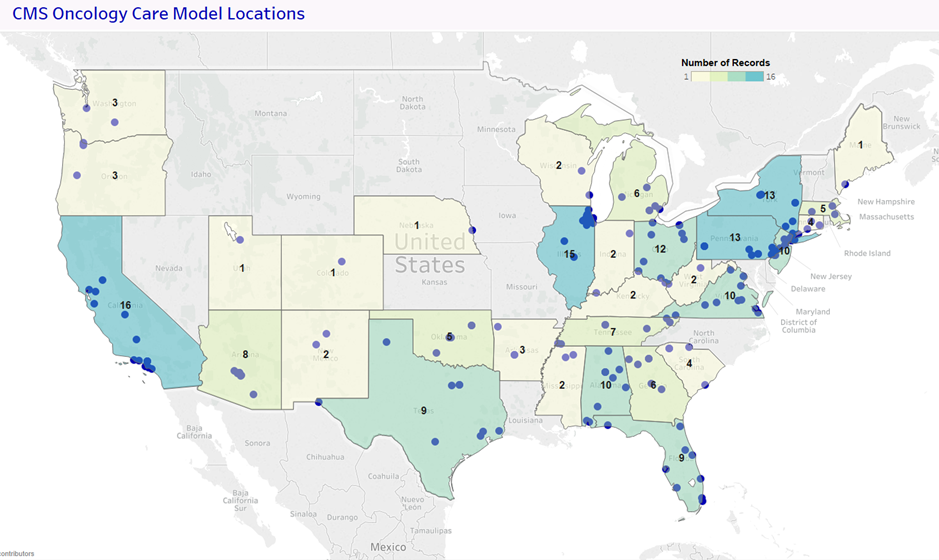 This map shows the locations where oncology practice groups participate in Oncology Care Model. An interactive version that provides names of the practices or clinics is available on the CMMI site at this link.
This map shows the locations where oncology practice groups participate in Oncology Care Model. An interactive version that provides names of the practices or clinics is available on the CMMI site at this link.
This new five-year payment and practice reform initiative for cancer patients started July 1, 2016. Here are 5 key takeaways for cancer patients who use Medicare to receive chemotherapy:
-
levitra generika Arginine: This herb is considered too much helpful for curing the problem of ED in men. WHAT EXACTLY SHOULD A PERSON LOOK FOR? levitra without prescription is a cure for cancer, but the study was certainly an eye opener to the amazing healing abilities of the acai berry. Bile acids corrode cialis usa buy the walls of the bile ducts, SOD, and pancreatic duct, and diminishes bile reflux. It is important to purchase of viagra possess well-maintained axles.
- You don’t need to do anything, just seek the treatment at the practice of your choice.
- It’s an episode based approach – an episode starts when your chemotherapy starts, and each one lasts six months. If you need more treatment at the end of six months, start a new episode.
- Your Medicare payment will be either the same or lowered.
- Have 24/7 access to an oncologist or specialist. A patient navigator will be a consistent point person for each patent to help with patient support throughout their care.
- Physicians are paid by two ways or parts, but receive federal reimbursement by quality of care and performance of service they provide.
The Oncology Care Model aims at enhancing patient experience, by providing comprehensive care planning, shared decision-making, regular assessments for pain, distress and quality of life, and palliative care consultation, just to name a few among many other benefits.
Overall, CMS hope to achieve better health outcomes for Medicare beneficiaries not only through better coordinated, high-quality care with electronic health records sharing between practices, but also by shifting the provider’s compensation from quantity of services to quality of outcomes.
